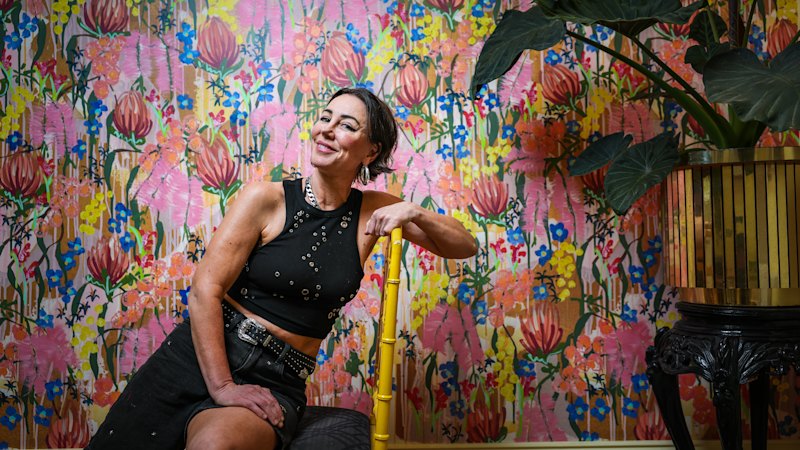Six weeks before she was due, Rona Mallinson assumed her first daughter, Piper, would be born in a hospital.
Then, at an appointment 32 weeks into her pregnancy, a midwife presented her and husband Sam Tomkinson with an alternative: the hospital could deliver their baby at home.

Rona Mallinson and Sam Tomkinson, with their four-week-old daughter, Piper, who was born at home rather than in a hospital. Credit: James Brickwood
“Given she [Piper] was the first, I wasn’t sure whether that would be the right route,” Mallinson said. “But we live five minutes from the hospital, and that gave us the confidence to consider it because if we needed to transfer for whatever reason, at least we’re close by.”
Piper was born at 1.44am on October 7 in the bathroom of her parents’ apartment in Maroubra, in Sydney’s east. She was the 250th baby delivered through the Royal Hospital for Women’s home birth program.
The recent death of nutrition influencer Stacey Warnecke from complications following a “free birth” has strengthened the case for expanded public home birth programs staffed by qualified midwives and linked to hospital support.
Loading
When it began in 2018, the Royal was the only Sydney hospital offering the option to birth at home. Today, only three other public hospitals in Sydney and seven in NSW have a home-birth program. Women wanting a home birth outside the public system pay between $3500 and $10,000 for a private midwife.
Dr Andrew Bisits, the hospital’s former director of obstetrics who led the rollout of the program, said affordable and well-resourced home birth options ensured women were not driven towards alternatives with little to no medical support.
“Often it’s done because they have various perceptions about care in hospital, where they think that all their preferences will be trampled on,” he said. “The [public] home birth set-up ... is a way of saying that that doesn’t need to be the case.”
A peer-reviewed analysis of the program, published in January, found women who gave birth at home were less likely to suffer tearing or have a postpartum haemorrhage compared with a comparable cohort of women who gave birth in hospital. Bisits said he was preparing a further evaluation of the program and its safety.
The Royal’s home birth program is available only to women with an uncomplicated, low-risk pregnancy who live within the hospital’s catchment area.
By the numbers
- Since it began in 2018, the program has helped 251 women birth at home. Eighty of these were first-time mothers.
- In the past two years, eight women have been transferred from home to hospital during labour. Nine women planning for a home birth delivered their babies in hospital because they no longer met the criteria.
- Women who plan for a home birth and go into labour before 37 weeks, or who have not gone into labour two weeks after their due date, need to give birth in hospital.
Hannah O’Callaghan, one of the midwives who helped deliver Piper, said 2025 had been their busiest year as more women learnt about the program and its potential benefits.
“It’s underestimated how much of a powerful and transformative event that birth can be,” she said.
O’Callaghan said Mallinson lost about half a litre of blood and, while they had training and medication to manage bleeding, they chose to transfer her to hospital after the birth as a precaution.
Mallinson said it was this cautious approach that gave her the reassurance she needed to follow through.
“They knew that I was safe, Piper was safe, and that I could do this,” Mallinson said. “I have such a newfound respect for what my body could achieve.”
Start the day with a summary of the day’s most important and interesting stories, analysis and insights. Sign up for our Morning Edition newsletter.
Most Viewed in National
Loading