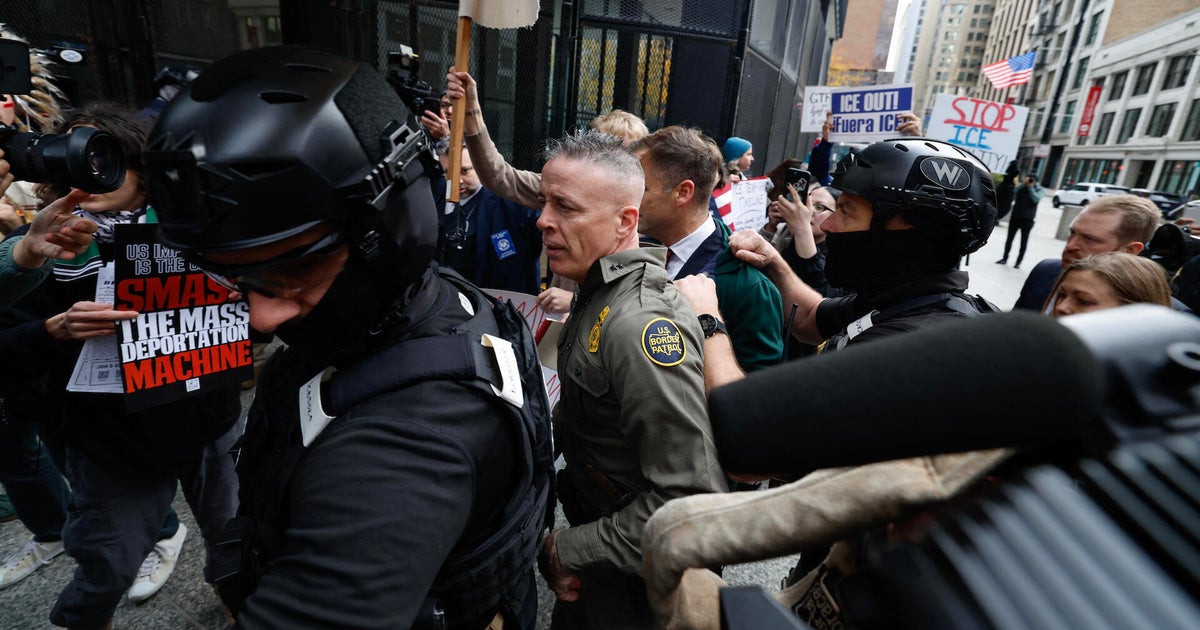There’s a question on Professor Kate Drummond’s mind. “How do people, after I’ve just told them: you might die, you might have a stroke, all these terrible things might happen … how do they lie there and just let someone put them to sleep?” she asks. “How are they not screaming?”
If you were going to trust anyone to poke around in your brain, you would struggle to find someone more qualified to do so than Drummond. She is the director of neurosurgery at the Royal Melbourne Hospital, has published more than 180 papers on the biology and management of brain tumours, and has pioneered awake surgeries for patients with the most severe forms of brain cancer.
It’s a question I should be able to answer. Five years ago, on Christmas Eve, 2020, my lunch companion removed a chunk of my brain after a two-month odyssey to find an explanation for the strange tremors in my left arm. Drummond had explained the risks; I could lose the use of my left arm and leg, and there was a chance I wouldn’t get it back. But the alternative wasn’t appealing either.

Health reporter Angus Thomson with Professor Kate Drummond, director of neurosurgery at the Royal Melbourne Hospital. Credit: Simon Schluter
The tremors had begun in my hand; the ring and the little finger, twitching as if pulled by invisible strings. When they progressed into full arm convulsions, an MRI confirmed the culprit: a non-cancerous, raspberry-sized formation of blood vessels called a cavernoma. Within two weeks I had an appointment with one of Drummond’s neurosurgical colleagues at the Royal Melbourne, who gave me two options: take anticonvulsant medication for the rest of my life, or get it removed for good.
“You were very clear that you didn’t want to be on tablets for your whole life,” Drummond recalls. The last time we spoke face-to-face, she was at the end of my hospital bed. I couldn’t move my left side. I could barely finish a sentence.
“We knew this would happen,” I remember her saying, but no amount of reassurance prepares you for the terror of waking up to find you can’t wriggle your toes; that you can’t pick up a fork even if you want to ingest the anonymous slab of meat wobbling about your hospital tray (I haven’t eaten turkey since).
Now we’re sitting in the window of Bar Lourinha, a cosy tapas bar in Melbourne’s CBD that has been a favourite of Drummond’s for two decades. The food beats Christmas lunch in hospital, and Drummond chats with the wait staff like old friends. She remembers the first time she came here (in 2006) because she had just bought Gotye’s Like Drawing Blood vinyl record, which they played for her behind the bar. It’s somewhere she likes to bring visitors, especially from overseas. “It’s pretty Melbourne,” she says. “Small, funky, weird.” We’ve both ordered the lunch rapido, a three-course seasonal chef’s menu. I go for the fried sardines with salsa picante, Drummond the roasted mushrooms.

Roasted mushrooms at Bar Lourinha.Credit: Simon Schluter
In a profession known for being hyper-competitive, blokey and, sometimes, a little impersonal, Drummond is none of those things. She decided to pursue medicine three months before her final exams at Hornsby Girls’ High School. “I’m not one of those people who had this lifelong ambition,” she says. “No one in my family had even been to university.”
All she knew was that she wanted to study at the University of Sydney. After 9-to-5 classes, she worked as a seamstress for a fashion designer, then in a bar. In her fourth year of medicine, she got married to an apprentice plumber, and moved into a unit in Parramatta close to clinical school at Westmead Hospital. She thought she wanted to be an obstetrician. “Then I delivered a baby, and I said I’m never doing that ever again,” she says.
During a junior neurosurgery rotation in her intern year, she met a young woman with a rare noncancerous tumour near her pituitary gland that was interfering with hormones and sending her blind. “I thought, ‘this is terrible. Someone really needs to care for this person’,” Drummond says. “At that time, I really had no qualifications to do anything for her, other than be nice to her on the ward and look after the general things.”

The fried sardines with salsa picante.Credit: Simon Schluter
She was hooked. “A lot of surgery is very ...,” she pauses. “Transactional is not the right word, but you see something, you fix it, it goes away.” Neurosurgery is different. For people with complex brain tumours or trauma injuries, their neurosurgeon can be part of their life for years. “And there’s a lot of medicine involved,” she says, again using my example. “Even for you, we had to get your seizures under control, you had all these other things that we had to look after … that’s what I really like about it.”
Drummond trained at Westmead for two years, a year at Royal North Shore, then six months each at Melbourne’s Children’s and Austin hospitals. She first arrived at the Royal Melbourne in 1997 to undertake research, and was supposed to go back to Westmead. “But I enjoyed Melbourne too much,” she says. “So I never went home.” She lives in an apartment near the hospital with her second husband, Jeff, a retired hot air balloon pilot who she met on a tour in Kenya (he was the pilot).
Melbourne might be their base, but hers is an international career. There’s a Boston Red Sox pennant hanging in her office, a memento from her two stints in the Massachusetts capital (once before and once after two planes hijacked from the city’s airport collided with the twin towers). When I emailed her in October to see if she would be interested in an interview, she was in Malawi, where she travels every year with a group of about 30 others in her role leading Pangea Global Health Education.
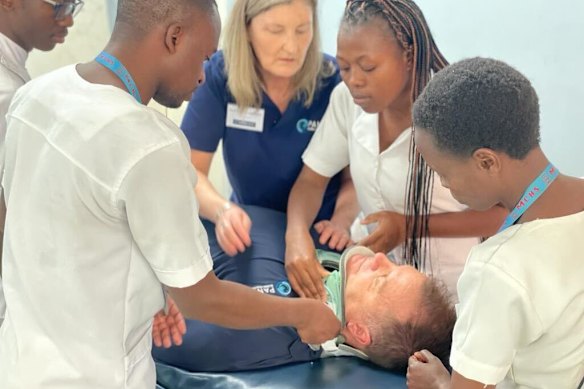
Drummond in Malawi.Credit:
The aim is not to treat patients directly but to build the skills of local health workers, from the basics of trauma surgery to how to phone a doctor in an emergency. “There’s a lot of people who go and work overseas, do a bunch of … stupid operations, stuff that is appropriate in our context, but not appropriate in that context, and wastes a lot of money,” she says. “I’d done a couple of things where I thought I was not particularly useful … and then this opportunity came up.” A nurse who participated in the program now teaches others. One of the neurosurgeons from Malawi will take up a year-long fellowship at the Royal Melbourne next year.
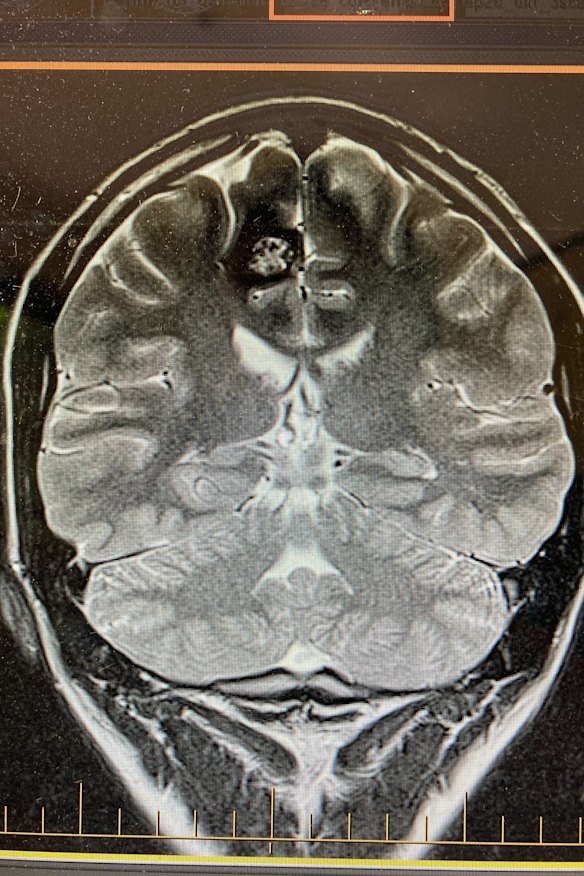
A scan of Angus Thomson’s brain showing the cavernoma at top left, which was causing his hand to shake uncontrollably.Credit:
Drummond would have come to lunch in jeans and a T-shirt, but has instead come dressed for church; Melbourne’s new Anglican Archbishop Ric Thorpe is being installed at St Paul’s Cathedral, and she is part of the ceremony. Faith has been a constant in Drummond’s life; she was adopted through an Anglican adoption service as a two-year-old. It has helped her through difficult times. When she returned from Boston in 2004, single and with no money, she did an hour a day of prayer and meditation, and an hour a week of spiritual direction with a trained guide, as part of the spiritual exercises of St Ignatius.
“You spend a year and a half examining your life for an hour a day, which is quite helpful, whether you frame it as a religious thing or whether you frame it as a spiritual thing,” she says. “I made a very clear decision that I was in the right place with my career.”
It’s something that she will often talk about with patients, but only if they ask. Some ask her to pray with them. “I’m not one of those people who go in and say, ‘don’t worry, Jesus will look after you’,” she says. “But for many patients, it’s a time in their life where they’re open to conversations like that.” Once she winds down clinical work, she wants to do a doctorate of philosophy on the theology of dying. But Drummond, who has held academic and teaching positions at the University of Melbourne for the best part of 20 years, got a rude shock when she proposed the idea to the dean of Trinity, the theology college. “He said, ‘Professor, you’re actually not qualified to do a humanities PhD’,” she laughs. She’s since finished a graduate diploma in theology.
We’ve been talking for two hours when our waiter politely asks if we can relocate to make room for the Sunday flamenco band. He brings us coffees, and now it’s the doctor’s turn to ask questions of the patient. “Are you still on anticonvulsants?” No. Any weakness? None – I recovered my fine motor skills after four patient months of rehab. The titanium screws in my skull don’t set off the airport metal detector. If I had a little more hair on my head to cover the thin white line across the top of my head, I could pretend the whole thing never happened. “It’s a very good scar,” Drummond says, allowing herself some pride in her scalpel work.

The bill.Credit: Nine
It’s only as we leave that I realise this must also be comforting for Drummond. When she operated, I was a 22-year-old journalism student terrified about what my diagnosis would mean for my career, my independence.
Now, I tell her, the most remarkable thing is that I barely think about it all. That is testament to the strength of our public health system (I paid more for the $10 post-surgery buzzcut), but also to the skill and dedication of people such as Drummond and the doctors, nurses, physiotherapists and speech pathologists who help teach your brain to work again.
I make a promise to let her know what I’m doing in another five years’ time. We shake hands. She heads south to the cathedral.