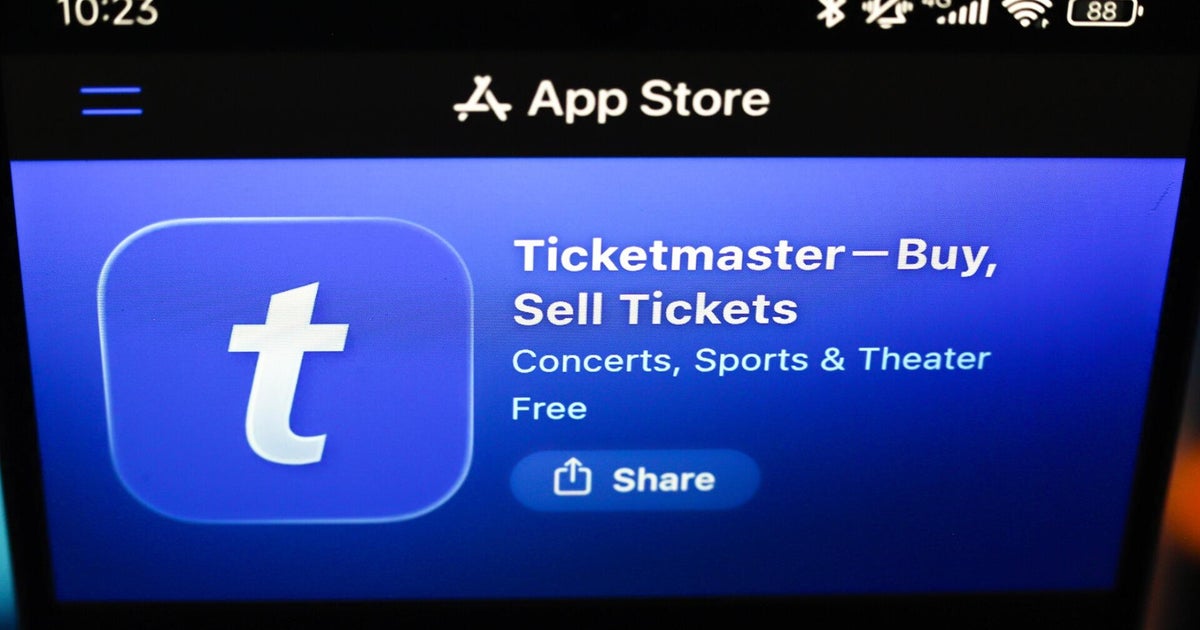
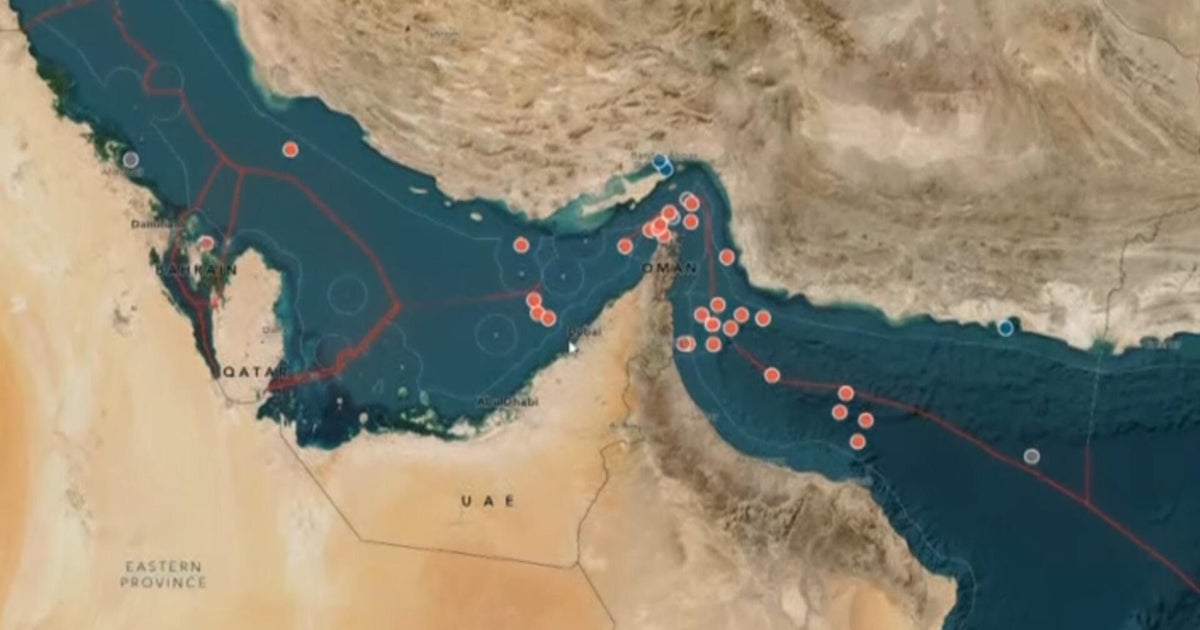
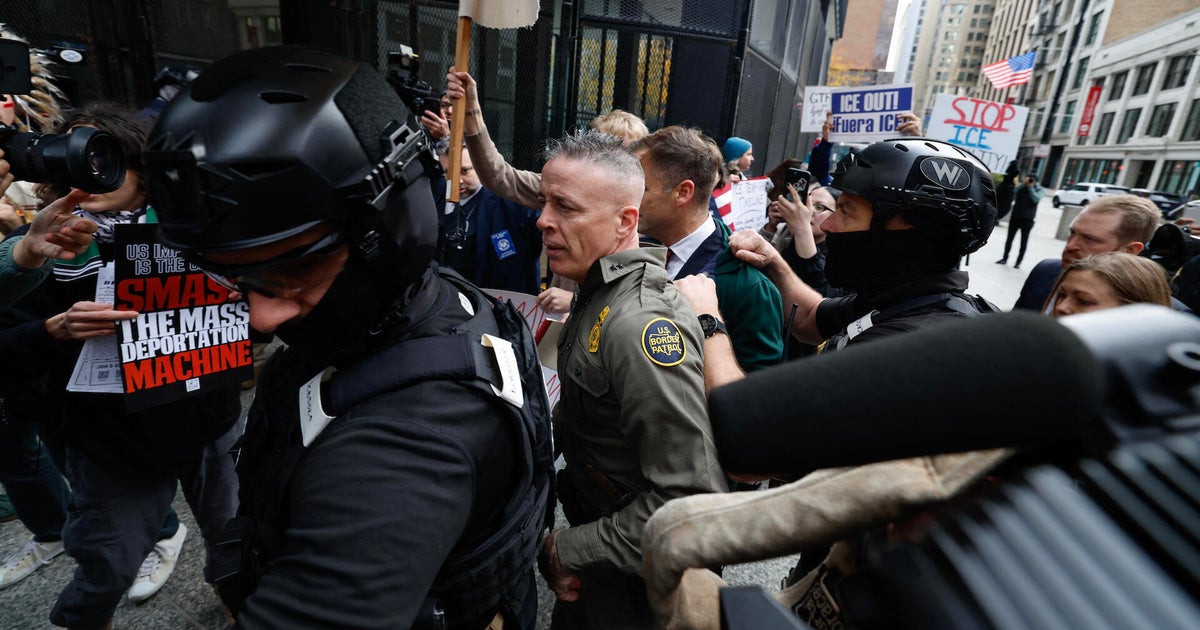Olga Gutteres sits ensconced in her patterned pink skirt, an island of colour at the centre of white hospital sheets. She stares out the window at the grounds of Dili’s Guido Valadares National Hospital.
A medical file at her bed’s end reads “suspected cervical cancer”.
Weeks later, laboratory results confirm the diagnosis. There is nothing “suspect” about it. The mother of eight (six living children) has cervical cancer that is too far progressed to be treated here, in Timor-Leste.
There is something perverse about an almost entirely preventable cancer killing young women, leaving children motherless in their most formative years and causing devastating intergenerational damage. An 85-minute flight south, Australia is projected to be the first country to eliminate the disease by 2035.

Olga Gutteres, 42, in the gynaecology unit ward where she has been diagnosed with advanced cervical cancer. Credit: Kate Geraghty
A “Junta Medica”, a committee of doctors, will determine whether Olga can be sent to Malaysia or Indonesia for treatment. But she has no passport or birth certificate.
“I need to return home to complete my documents,” Olga says. “I’m worried if I can do all this, to complete these things … and I am sad because I have many children,” she says, tears dropping into her lap.
In another room of the hospital’s gynaecology ward, Maia Domingas also has suspected cervical cancer. Stage 3, according to her file. The 38-year-old mother of three needs treatment overseas, but has no passport.
It has been vanishingly rare for doctors in Timor-Leste to encounter women with early-stage cervical cancer, the second-most common cancer for women in the country. It is a killer, with a mortality rate more than four and a half times that of Australia. For too many with later-stage cervical cancer, their only option is palliative care, and access to adequate pain relief is no certainty.

Maia Domingas, 38, has advanced cervical cancer and lies in the gynaecology unit ward waiting to see if she is eligible for treatment overseas. Credit: Kate Geraghty
“My doctors have said good things to me,” Olga says. “Encouraging me to continue to follow the Bible and pray hard to my Jesus so that I can return to good health.”
Gynaecologist Dr “Zeto” José António Gusmão Guterres has heard enough.
“This is what it means to have cervical cancer in this country,” Zeto says, shattering the unsteady rhythm of Olga’s softly spoken Tetum and his English translation.
“I’m sorry, I cannot interpret any more.”
Behind Zeto’s glasses, his face is wet.
90-70-90
Cervical cancer is a major public health issue in the Indo-Pacific, where, in some countries, women are up to 14 times more likely to die of the disease than in Australia. A tenacious team led by cancer-quelling experts is leveraging Australia’s elimination breakthroughs across the region.
The Elimination Partnership of the Indo-Pacific for Cervical Cancer (EPICC) is a four-year, $35.1 million program funded by the Australian government ($22 million) and Andrew and Nicola Forrest’s Minderoo Foundation ($13.1 million).
Led by the University of Sydney, the EPICC project supports health ministries across the region, including Papua New Guinea, Indonesia, Vanuatu, Fiji, Malaysia and Solomon Islands, in a three-pronged attack.
“This is about getting to 90-70-90 by 2030,” said Professor Karen Canfell, a pioneer in elimination efforts, and EPICC lead at the University of Sydney’s Cancer Elimination Collaboration (CEC).

Professor Karen Canfell, a pioneer in medicine and leader of the EPICC consortium at the University of Sydney’s Cancer Elimination Collaboration.Credit: Kate Geraghty
What sounds like an inadvisable padlock combination is the crux of the World Health Organisation’s ambitious cervical cancer elimination strategy.
EPICC is the only program working across all three pillars, Canfell said. With an international consortium, including the Australian Centre for the Prevention of Cervical Cancer, The Kirby Institute (UNSW), Family Planning Australia, and UNITAID, the program draws on dozens of experts across all crucial components.
“That’s everything from HPV vaccination at school and in the community, HPV screening and treatment, improving oncology services, and even palliative care and pain relief … We try to meet the country where it’s at.
“It’s about protecting girls and women at every stage,” the cancer epidemiologist said. “We could save 62 million lives in low and middle-income countries over the century by eliminating cervical cancer.” (Elimination is defined as fewer than four new cases per 100,000 women per year.)
Australia has led the world in cervical cancer elimination
Australian immunologist Professor Ian Frazer co-developed the first cervical cancer HPV vaccine (Gardasil) in 1991 with Chinese virologist Dr Jian Zhou at the University of Queensland.
That same year, Australia became the first country to implement national cervical cancer screening, and in 2007, Australia launched a world-first national HPV immunisation program.
Australia was also among the first countries to switch to HPV screening in 2017 and self-collection in 2022.
The team must navigate labyrinthine bureaucracies and counter stigmas and superstitions that favour traditional healers offering pastes, herbs, and tinctures over modern medicine.
In Timor-Leste, EPICC has canny allies. From DFAT embassy staff, government ministers, and the health ministry, to passionate healthcare workers, Catholic archbishops, priests, and local chiefs in this deeply devout and fiercely independent half-island nation.
The clinic
Olinda*, 35, sits in a consultation room of the Vera Cruz Community Health Clinic. It’s the site of Timor-Leste’s first HPV cervical cancer screen-and-treat service that enables women to self-collect samples. No speculum and pelvic exam.
The samples are tested in-clinic using a portable molecular diagnostics machine, a lab-in-a-box the size of an air fryer. Women get their results one to two hours later.
Almost every sexually active person will have an HPV infection at some point. But only a handful of the 200 known HPV strains are linked to abnormal cell changes that increase the risk of cervical cancer (and some other cancers of the genitals, anus, head and neck in men and women).
The heavy-hitters are HPV 16 and HPV 18, which cause more than 70 per cent of cervical cancers worldwide.

Dr Maria Jose consults with Luisa before she self-tests for the human papillomavirus (HPV) at the Vera Cruz Community Health Centre in Dili.Credit: Kate Geraghty
Roughly 13 per cent of women who come through the service at Vera Cruz will test positive for cancer-causing HPV types. Olinda is among them.
She seems calm, even laughing as Dr Maria Jose explains she has an “intermediate risk” HPV type and shows a diagram of a cervix with precancerous lesions.
Behind Olinda on the consulting room wall is a calendar, where under today’s date someone has written “Deb’s Back!”
Deborah Bateson, Professor of Practice and EPICC’s deputy lead at the CEC, is indeed in Dili to, as she puts it, “do myself out of a job”.
“We need to make ourselves redundant by supporting countries with the training and resources to continue this work.”
It’s also about proving the interventions are sustainable and pay dividends in national productivity while saving women’s lives.

Deborah Bateson, EPICC deputy lead and Professor of Practice at University of Sydney Faculty of Medicine and Health, at the foreshore in Dili.Credit: Kate Geraghty
“Everyone you meet in Timor knows someone with cervical cancer or someone who has died of this terrible disease, often horrible deaths, stigmatised and isolated,” Bateson says.
“Screening women is absolutely critical to successful elimination. It’s also helpful for raising awareness of the symptoms … vaginal bleeding and pelvic pain, for women who feel too ashamed to seek help.”
Ana* is waiting in the clinic hallway to be screened.
“In my mum’s time, cancer was [believed to be] a curse … People with cancer were separated and isolated,” the 45-year-old said. “You were told to stay away from them. It was very sad.”
Ana took time off work for the screening and hopes to convince her female colleagues to come in. “They are shy,” she said. “But this is so very important.”
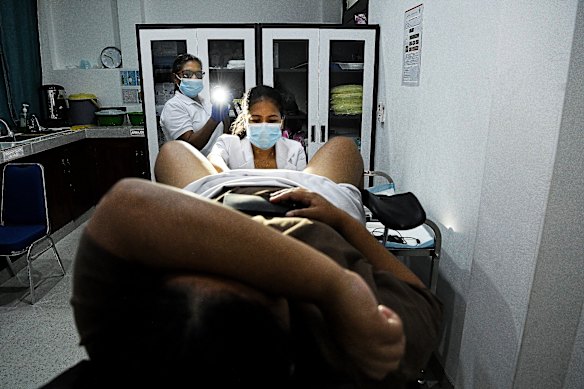
Olinda, 35, undergoes thermal ablation treatment after testing positive for HPV.Credit: Kate Geraghty
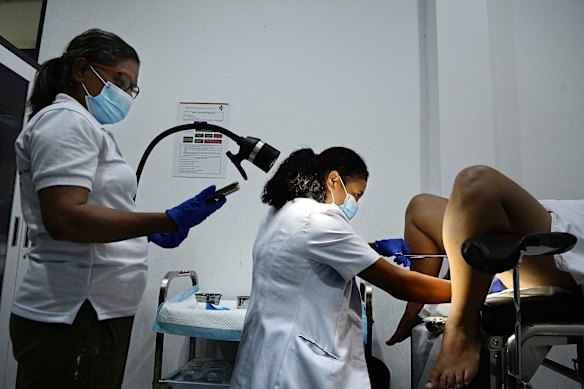
Dr Maria Jose GP (right) performs the thermal ablation treatment, assisted by midwife Filomena Mendonca Espirito Santo, at the Vera Cruz community health centre.Credit: Kate Geraghty
Olinda lies on an examination bed as Dr Maria applies a swab of acetic acid to her cervix. Any precancerous lesions will whiten on contact. Olinda is eligible for thermal ablation, where Dr Maria uses a wand-like probe heated to about 100 degrees to destroy abnormal cervical cells. The procedure, which takes a few minutes, is only mildly uncomfortable, Olinda says.
Leave no woman behind
Since March, more than 1000 women aged 30 to 49 have been screened through this service, and more than 110 treated.
“There was nothing like this here before,” says Dr Adriano Pereira, known as Dr Andi, EPICC’s in-country project co-ordinator.

EPICC’s in-country project co-ordinator Dr Andriano Pereira in the testing laboratory at the Vera Cruz community health centre.Credit: KATE GERAGHTY
“The bishops and priests are really on board,” he said. “[During their Sunday services], they will encourage women to come in for cervical cancer screening.”
Such an endorsement is hitting the public health promotion lottery in a country where 97-98 per cent of the population is Catholic.
In two days, EPICC staff will travel to the Dili suco (village) of Vila Verde for a routine outreach event alongside public health initiatives. With the suco chief’s blessing, an ambulance with a loudspeaker mounted on the roof roams the streets of Vila Verde, calling on women to come along. The clinic staff screens 43 women on the day.
That week, EPICC helped run a gender equality, disability and social inclusion workshop with members of Timor-Leste’s LGBTQ communities, sex workers, and disability and gender equity advocates to develop strategies for reaching marginalised women.

Professor Deborah Bateson (second left) talks with EPICC midwife Filomena Mendonca Espírito Santo at a medical outreach event in Vila Verde village.Credit: Kate Geraghty

A Timorese woman waits to use the toilet to self-test for HPV at the outreach event.Credit: KATE GERAGHTY
The initial aim is to screen 5000 of the roughly 161,000 eligible women in Timor-Leste. After EPICC helped procure the necessary tests and equipment, develop the screening algorithm and guidelines, and upskilled healthcare workers, the Ministry of Health plans to expand the program.
“We are not going to leave any woman behind,” says Dr Andi, named after a doctor who treated civilians during Indonesia’s December 1975 invasion.

University of Sydney medical oncologist Dr Telma Costa greets people at the Pakote Integradu Saude outreach event in Vila Verde village.Credit: KATE GERAGHTY
Dr Telma Costa, oncologist and EPICC Timor-Leste program manager, recalled a virtual meeting with Andi during an earthquake. During a common wet season flood at the Ministry of Health, Andi worked in knee-deep water.
“They are amazing,” Costa said of Andi and his fellow health professionals working with EPICC. “It’s so hard to do what they do with so little and to keep motivated, caring and attending calls and having ‘the Australian team’ wanting to have virtual meetings with terrible internet.”
Last year, Timor-Leste vaccinated 56,350 11- to 14-year-old school girls – 90 per cent of this target population – during the country’s first HPV immunisation drive, according to health ministry figures.
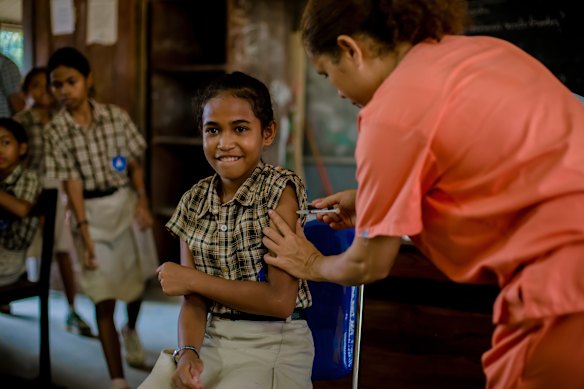
School student Nofelia Maia da Costa Belo Lopes (centre) receives the HPV vaccination at the Rumbia Primary school in Dili.Credit: Rey Marques

Rumbia Primary school students Riana, Dolores and Felizarda are among those waiting to receive the HPV vaccination.Credit: Ray Marques
EPICC partner the National Centre for Immunisation Research and Surveillance provided technical assistance for the initial rollout, and annual HPV vaccination is now in the country’s routine immunisation program.
In 15 to 20 years, when these girls are Olga and Maia’s age, the pay-off will be a dramatic decrease in cervical cancer cases.
Generations of elimination
“All she wants to do is dance all day,” Filomena Pereira Ekuttan says as we watch her four-year-old daughter, Grace, mimicking a viral TikTok routine.
Grace kicks up the loose earth of the family cemetery in Batugade, near Timor-Leste’s border with Indonesia.
The grave of Filomena’s mother, Maria de Encarnacao, is shielded from the sun and monsoon rains by an aluminium canopy.

Filomena Zennefer Pereira Ekuttan, 24, and her daughter Grace, 4, at her mother’s grave near Batugade village. Maria de Encarnacao Pereira died of cervical cancer.Credit: Kate Geraghty
Maria was a nurse, but waited roughly six years to see a doctor for her abnormal bleeding and back pain.
“She did not know these were symptoms of cervical cancer,” Filomena, 24, said.
Maria had chemotherapy and radiation therapy in Kuala Lumpur. She was given the all-clear, but within two months her pain returned. On a Chinese naval ship in Dili, she was diagnosed with advanced cervical cancer. More treatment in Malaysia was futile. She died three months later in March 2024.
“I have learnt all I can about cervical cancer … I know we can prevent it,” Filomena said. “My dream is to get Grace vaccinated, and for myself to be screened.”

Timorese students walk along the main road in Balibo. In 2024 the government of Timor-Leste launched a single-dose HPV vaccination program for girls aged 11-14 years. Cervical cancer is the second-most common cancer among women in Timor-Leste. Credit: Kate Geraghty
Screening will find more women with cancer, a problem for a healthcare system with few treatment options beyond surgery for early-stage cases, and a healthcare budget already spending millions to send cancer patients overseas for chemo and radiation treatment.
It was a dilemma Dr Flávio Brandão Mendes de Araújo, Vice Minister of Health for Hospital Operationalisation, raised when he first met with Bateson and Costa in 2023.
“We need to find the cases, but we also need to be able to treat the cases we find,” he said.

Dr Flavio Brandao Mendes de Araujo at his office in Dili, Timor-Leste.Credit: Kate Geraghty
“Some of the highest rates of sending patients overseas are cervical cancer patients. I hope that through collaboration with EPICC, we can [offer] more services.”
Costa said in future, EPICC will support Timor-Leste with broader treatment options. But first, the hospital must have the capabilities for timely diagnosis and staging.
The lab
At the back of the National Hospital’s laboratory is floor-to-ceiling shelving crammed with biopsy samples: bulbs of tissue and tumour suspended like jellyfish in jars of viscous fluid with handwritten labels.
The specimens would be medical waste in Australia, but preserving them is a kindness.
“I keep them for the families,” Dr Odília Carvalho, head of the pathology laboratory, says. “When someone dies, sometimes the family comes here and asks to bring them home for cultural [rituals].”
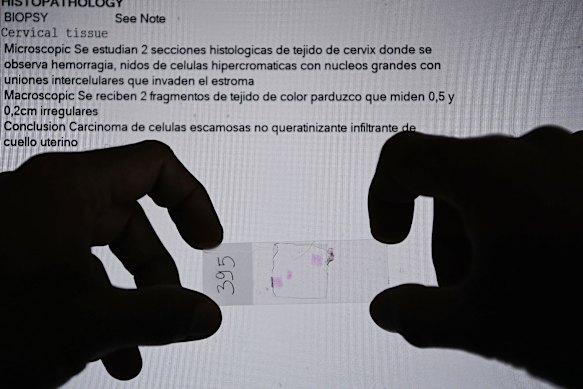
Guido Valadares National Hospital histopathology laboratory unit technician Nelson Tonito Marcal Sequeira holds a patient’s cervical cancer sample. Credit: Kate Geraghty
EPICC has been upgrading and replacing equipment in the histopathology laboratory (the gold-standard technique for cancer diagnosis), as well as training and mentoring staff.
Laboratory technician Nelson Tonito Marçal Sequeira and four other Timorese health professionals (an oncologist, two gynaecologists, and a midwife) secured EPICC Australia Awards Fellowships to strengthen their skills and leadership, including a two-week training program in Sydney.
“It was a nice way to start building a multidisciplinary team approach to cervical cancer in Timor-Leste,” Costa said.
It’s not unusual for the lab to run out of reagents – the chemicals used to prepare tissue samples. The pathology oven, used to thaw samples, is old, Sequeira says. He leads Bateson to an automatic tissue processor and shows her several broken reagent containers.
“Part of our work is making sure that you’re not leaving expensive equipment that no one can service, or there are no spare parts [available] and it all breaks down,” Bateson says.
‘I can’t experience women dying’
“When EPICC comes in,” Zeto says, “I feel this is a dream come true for me as a doctor.”
We are back at the national hospital with the gynaecologist, this time in a vacant room with glass-panelled doors, wallpapered with blue skies and yellow hot-air balloons.
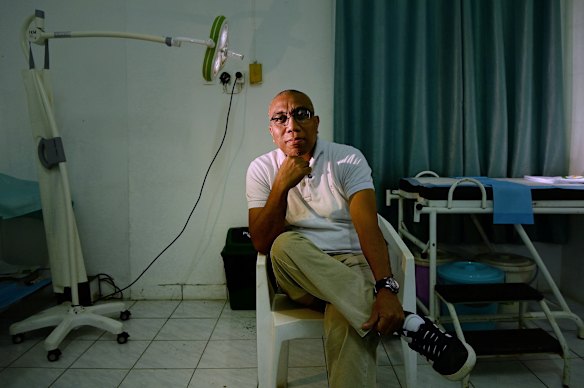
Dr “Zeto”, gynaecologist José António Gusmão Guterres, at the Guido Valadares National Hospital in Dili.Credit: KATE GERAGHTY
By early 2026, this will be the site of a preinvasive lesion clinic – another EPICC initiative – staffed by health practitioners trained to diagnose and treat women who are not eligible for thermal ablation (for instance, their precancerous lesions are too large, too deep, or suspicious for invasive cancer).
A more powerful colposcope – a specialised lighted microscope – arrived in October, and the clinic will be able to offer a procedure called Large Loop Excision of the Transformation Zone to remove pre-invasive cells.
“I take it very personal[ly] because I can’t experience women dying [any more],” Zeto says, recalling the years in which he never saw a woman with early-stage cervical cancer.
“They would all come too late. When I talk to the women … the husband and the kids … You can’t imagine how deep is the feeling, the sadness, the frustration [they] are facing.”
Zeto, an EPICC fellow, has seen the inside of a Liverpool Hospital operating room, the resourcing of Australia’s system and the clinical outcomes data for Australian patients, where mortality rates are one-fifth of Timor-Leste’s.
“I hope this is not something that will emotionally trigger you, then you go away and do something else,” Zeto says.
This cynicism is understandable, Canfell says. Timorese doctors have seen aid groups arrive, set up, then leave when funding dries up.
Among the bright facades of Dili’s Portuguese colonial architecture are half-constructed skeletons of concrete and steel rods of aid projects financed then abandoned by foreign investment – mausoleums of soft diplomacy.

A family plays as the sun sets at the foreshore in Dili.Credit: KATE GERAGHTY
“It genuinely keeps us up at night, and it should,” Canfell says. “There has to be an enduring country-led program here. Otherwise, we are doing a disservice to the country.”
On the sidelines of the UN General Assembly in New York in September, EPICC and the Women’s Health and Economic Empowerment Network launched a $50 million technical assistance facility to coordinate sustainable blended public-private financing for non-communicable disease and women’s cancers. Its first project will be to eliminate cervical cancer in Indonesia.
EPICC is involved in validating new HPV test candidates and is expected to play a growing role in securing the best prices for vaccines and tests, Canfell said.
Foreign Minister Penny Wong said all women deserved to live a life “free from a disease we have the power to prevent”.
“It is not just the right thing to do – building a healthier, more stable and more prosperous Indo-Pacific is in Australia’s national interest.”
Minderoo Foundation chief executive John Hartman described EPICC as a transformative initiative with profound implications, not only for cervical cancer elimination but for entire healthcare systems. (Minderoo also provided $8.6 million for EPICC’s predecessor.)
“By investing in scalable, locally led solutions … we are helping to build resilient health systems and drive lasting change,” Hartman says.
Dignity in death
Under a red cedar tree on the USyd campus, Julia Da Costa describes the relentless screams of the colorectal cancer patient in a Timor-Leste hospital.
“All they gave him was tramadol,” Da Costa says. The weak opioid did not touch the sides of this man’s agony. “Most patients in pain don’t get opioids at all.”

University of Sydney PhD student Julia Da Costa is researching opioid access for pain management in Timor-Leste. Credit: Kate Geraghty
Bateson says improving palliative care is a crucial component of EPICC’s work.
“Screening is going to find more cervical cancers; and even if they are untreatable, women should be able to die with dignity,” she says.
“Julia’s work will be absolutely invaluable,” she adds, not just for cervical cancer patients, but all patients in pain.
Palliative care patients should have access to morphine and fentanyl, but many facilities do not stock them.
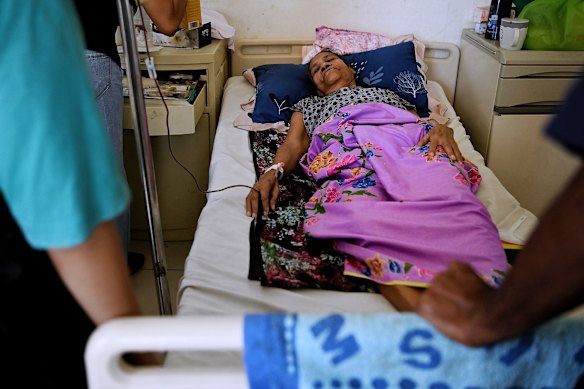
Colon cancer patient Joana Da Costa, 66, in palliative care unit of the Guido Valadares National Hospital. Credit: Kate Geraghty
Doctors said patients’ pain was well-controlled, but when Da Costa visited, “they were clearly suffering”.
Part of her PhD involves developing a policy and guidelines to improve access to opioids. It will provide the scaffolding for EPICC’s work.
“There is a lot of resilience in Timor. We’ve been through a lot, and there is this culture [around pain] that we should tough it out. No one complains,” she said.
“But no one should suffer.”
*Pseudonyms have been used in order for women to share personal medical details.
Aubusson and Geraghty travelled to Timor-Leste as guests of the University of Sydney and the EPICC team.