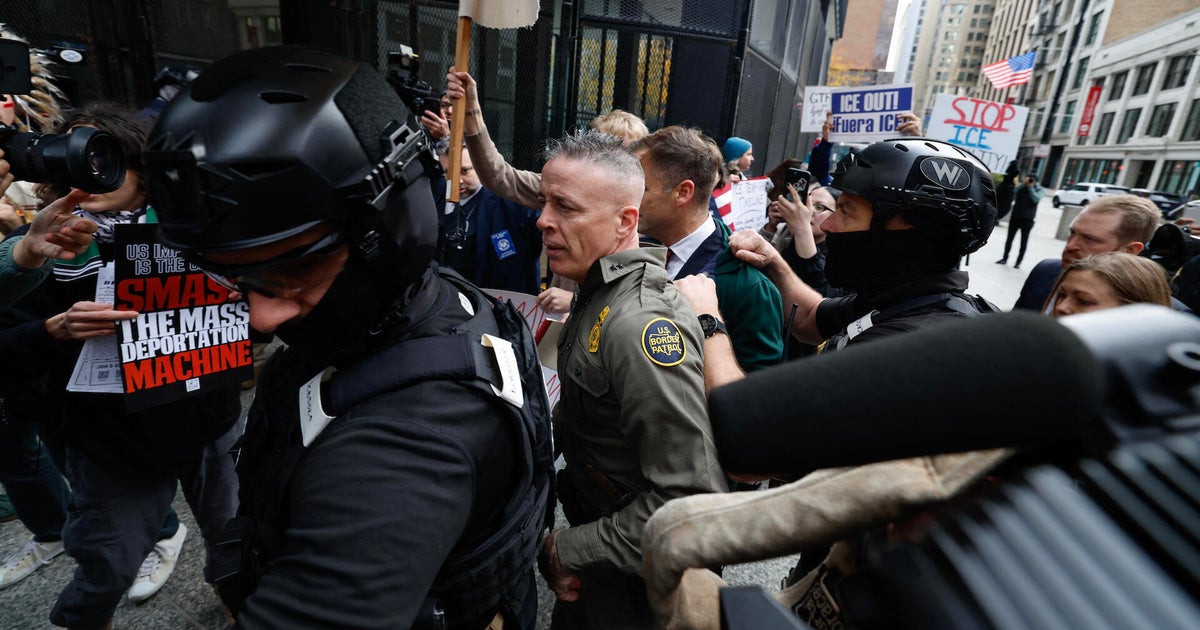Hope Island resident Bill Leavy had started to notice his memory slipping, but it wasn’t until an incident involving a handbag that he considered a more serious prognosis.
His wife, Jenny, had asked him to grab her bag from the kitchen bench. Leavy obliged, but found no handbag in sight. Jenny insisted otherwise.

Hope Island resident and Dementia Australia advocate Bill Leavy was diagnosed with Alzheimer’s disease in 2024. Credit: Courtney Kruk
“She got up and there it was,” Leavy explains. “Big white stone bench, beautiful big black handbag.
“I’m thinking, how did she sneak around and put it there, because it wasn’t there a moment ago.”
Leavy now understands the incident as a symptom of Alzheimer’s disease, a common form of dementia that affects memory, thinking and behaviour, with which he was diagnosed last year.
“It’s a misinterpretation,” he says. “My brain isn’t interpreting what my eyes can see.
“That happens a bit for me.”
Loading
Nearly half a million Australians live with dementia, a figure projected to double by 2058. A further 1.7 million are involved in their care.
But research shows people generally have a poor understanding of the condition and its characteristics, causes and symptoms.
“With dementia, the first thing that comes to mind for people is probably a little old man or lady sitting with a towel across their lap not knowing who’s there, just out of it,” Leavy says.
“There’s plenty of people like that, but there’s a lot more people like me and others that have been diagnosed [and are learning] to deal with this stuff on a daily basis.”
In the opening pages of her book What I Wish People Knew About Dementia, dementia advocate Wendy Mitchell wrote that when people thought of dementia, they immediately associated it with memory.
“Few people realise, for example, just how it changes our relationships with our senses, our emotions, our communication.”
Loading
Mitchell was 58 when she was diagnosed with early onset Alzheimer’s disease. It was an isolating experience, with limited information to understand her condition. So she started filling the gaps herself.
In interviews, Mitchell spoke about marble floors taking on a lake-like appearance, blank TV screens transforming into gaping black holes, and smelling smoke in the absence of fire.
Such sensory and perceptual changes are common for people living with dementia as the condition damages parts of the brain that interpret information from sense organs.
It’s why Leavy was unable to see his wife’s handbag on the bench, and why some people report struggling with certain surfaces, colours or shapes.
“Black mats on the floor are a worry for me,” Leavy says. “Not all the time, but sometimes I’ll see a mat, and I know it’s a mat, but I approach with trepidation.”
Hallucinations and delusions are also common, caused by the same misinterpretation of information in the brain.
Amanda O’Brien delivers dementia training for home carers at the Dovida Academy in Springwood. She switched from primary school teacher to aged care work after her mum was diagnosed with Alzheimer’s disease.
“I became passionate about wanting to raise awareness because there are so many misconceptions about dementia,” she says.
Dementia is an umbrella term to describe a range of neurological conditions affecting the brain over time. Credit: Getty Images
Dovida’s training includes a “simulation” for carers to better understand the challenges their clients face.
O’Brien begins the session by inviting participants to identify triggers – items such as a head-shaped lamp and sequinned pillows – that could be misinterpreted and in turn confusing for someone with dementia.
Pointing to the grey and black patchwork carpet and a curved indoor plant, she explains how colours and patterns lose their form.
“[The person with dementia] doesn’t know if that’s a person or somebody following them,” O’Brien says, gesturing to the shadow cast by the plant. “It can be quite scary.”
In the second part of the session, carers wear glasses covered with vaseline, thick rubber gloves and ear plugs to mimic cognitive challenges. The accessories make simple tasks such as shuffling a deck of cards, reading a food menu and tying shoelaces near impossible.
Loading
“People can think people with dementia are stupid or are going crazy because sometimes their behaviours can escalate,” O’Brien says.
“But we need to look at the bigger picture and ask why is their behaviour like that.”
Like Mitchell, Leavy found himself navigating lonely terrain after being diagnosed.
It’s why he became a Dementia Australia advocate and now speaks publicly, at schools and events, about the condition.
“Lack of information has always been the biggest problem,” Leavy says.
“And stigma – from other people and from ourselves because we don’t want people to think we’re stupid.
“I’m lucky. I’ve always been a confident young man and I don’t care what people think. So I quite openly talk about my dementia.”
Start the day with a summary of the day’s most important and interesting stories, analysis and insights. Sign up for our Morning Edition newsletter.