Mongolian shamans beat wicker drums to summon ancestral spirits. A Peruvian man in a headdress unleashes a piercing ululation. And a man from Kentucky tells me the body can rid itself of cancer if you eat the right shrubs.
It is a line-up one might expect at the healing field at Glastonbury, but this is a conference centre in New Delhi and the event has been organised by the World Health Organisation: the WHO Global Summit on Traditional Medicine. It’s the second gathering of its kind, following an inaugural meeting in Gujarat in 2023, and last month’s three-day event drew hundreds of delegates from around the world.
Alongside yoga instructors, aromatherapists, Chinese herbal practitioners and a small army of homeopaths sat senior WHO officials, leading scientists and health ministers from across Africa, Asia and Latin America. Only Gwyneth Paltrow and her wellness website Goop was missing.
They were there to “harness the potential” of traditional medicine, a catch-all term for practices that pre-date, and sit outside, modern evidence-based healthcare; therapies that for the most part have long been dismissed as quackery by mainstream science. What counts as “traditional medicine” ranges from drinking herbal teas to Indian Ayurveda, a holistic “wellness system” combining oils, herbs, homeopathy, yoga and meditation to “balance” and “heal” the body. To critics – and there are many – the scene was absurd.
So why is the WHO – a global authority on evidence-based health – giving a platform to this stuff? Has it fallen victim to the seductive power of TikTok-based wellness, like so many of the West’s middle classes? Or has it – as some critics allege – been bought off by the traditional medicine superpowers of India and China?
The organisation insists the summit is entirely legitimate. It is not about endorsement but “restoring balance” to the “science and practice of health and wellbeing”. Specifically, say its scientists, it’s about subjecting traditional medicine to the same scientific standards as modern medicine in order to, once and for all, separate the wheat from the chaff. Amid all the matcha lattes and essential oils, there could be life-saving cures, it says.
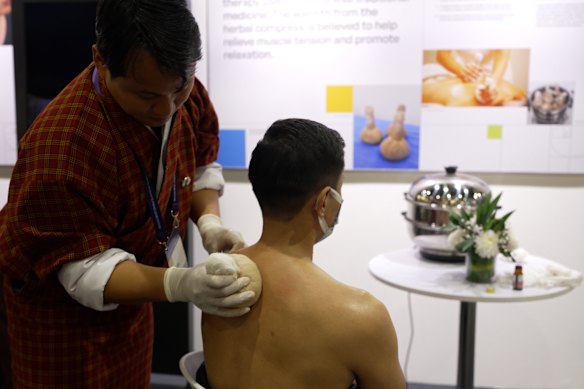
Nevertheless, delegates were invited to partake in sessions ranging from “intercultural expressions of healing” – in which spiritual leaders from Colombia present at the conference “reconnect participants with nature” – and a “Chingdug herbal compress experience” where guests are “detoxified” via Bhutanese herbs.

In the West, we like to think of ourselves as thoroughly science-based, but the truth is more nuanced. It was only in the late 19th century that germ theory started to replace the notion that disease was caused by miasma or bad air. Even then, it took almost another 100 years for the rigour of the scientific method to get a proper grip. Pioneers like Florence Nightingale and John Snow – both of whom used data rather than tradition to improve hygiene – did their bit, but real reform came much later.
The phrase “evidence-based medicine” – the doctrine that now dominates medical science in the West – was only coined in the early 1990s. And it was only in 2018 that the NHS closed its last homeopathic hospital. Through the application of scientific rigour, Western medicine has ruled out much quackery but also found hard evidence to support some traditional cures.
Aspirin is a prime example. It comes from willow bark, used some 3500 years ago by ancient Sumerians, Egyptians, Greeks and Romans to treat aches and fevers. In the early 1800s, a German chemist isolated its main active ingredient, salicin, and began prescribing it for pain relief. Yet it was only in the 1980s that it was definitively proven to work, not just for pain relief but as prevention against heart attacks, blood-clotting disorders and, more recently, certain cancers.
Other examples include acupuncture used for migraines and ginger used for nausea and vomiting in pregnancy.
The WHO says its summit on traditional medicine is essentially about repeating this sifting process for traditional remedies used in other parts of the world. It aims to apply rigorous scientific analysis to all of them to properly assess their claimed benefits and potential harms. By 2034, it says, it will publish a definitive list of which traditional treatments work – and which don’t.
“Working on traditional medicine doesn’t mean we will use shortcuts or endorse things that are unproven,” Dr Sylvie Briand, the WHO’s chief scientist, said at the conference. The aim was first to document what traditional treatments existed around the world “and then see what could be more useful to address the disease of this century”.
One idea is that some traditional practices like yoga and meditation, while perhaps not offering direct curative benefits, could play an important role in preventative medicine. After all, so-called non-communicable diseases, often caused by lifestyle factors such as poor diet, chronic stress and a lack of exercise, are now by far the biggest killers across the globe.
“Many traditional systems of medicine take a holistic view and focus on strengthening the person as a whole, not just treating isolated symptoms,” said Dr Sung Chol Kim, unit head for traditional, complementary and integrative medicine at the WHO.
But others are sceptical. They fear the WHO, which is struggling for funding in the wake of the US leaving the organisation and widespread aid cuts, is simply pandering to India and China where traditional medicine is big business. Even if well-intentioned, they worry that the discovery process the WHO has set in motion will end up promoting and legitimising quackery.
“I think highly of the WHO. However, by giving a platform to traditional medicine practitioners who promote treatments that are unproven – or even disproven – such as homeopathy, the organisation risks legitimising quackery. That, in my view, is both unethical and irresponsible,” said Dr Edzard Ernst, a British-German academic who specialises in the study of complementary and alternative medicine.
Certainly, the political forces at work at the WHO’s conference in Delhi are also difficult to miss. Chinese herbal medicine and Indian Ayurveda dominated proceedings, with large delegations from both countries invited to speak.
Ayurveda, meaning “knowledge of life,” is an ancient Indian holistic system of medicine which aims to balance mind and body through a mix of diet, herbs, yoga and meditation. It emphasises personalised care – which can’t be bad – but promises to “detoxify and harmonise the body’s unique energies for overall wellbeing”. For this there is little, if any, scientific evidence.
Patanjali, India’s largest Ayurvedic firm, has marketed products such as bottled cow urine, claiming it can treat eczema, diabetes and even cancer. Prime Minister Narendra Modi, an Ayurveda devotee, attended the conference as guest of honour and was repeatedly praised by senior WHO officials.
“I extend my deepest appreciation to the government and people of India – and in particular to Prime Minister Modi – for hosting this summit, and for his unwavering, continued leadership and partnership,” said WHO director-general Dr Tedros Adhanom Ghebreyesus in his closing remarks. “Through its centuries-old Ayush systems, India has shown the world that traditional wisdom and modern science are not inconsistent, but complementary,” he added.

Both China and India have invested heavily in promoting their medical traditions at home and abroad. India donated $350 million to establish a permanent WHO Global Centre for Traditional Medicine in Jamnagar in 2022 and largely funded the Delhi conference. China, meanwhile, has become the WHO’s single biggest funder now that the US has pulled out, promising investment of $US500 million over the next five years.
Herbal medicine is a multibillion-dollar industry in China and is used by at least 75 per cent of the population. While some elements of traditional Chinese medicine – such as acupuncture for chronic pain – have demonstrated benefit in clinical trials, large parts have also been debunked as pseudoscience. The use of animal products such as bear bile for pain relief and inflammation and rhino horn for everything from rheumatism and typhoid to “devil possession” do not just put patients at risk but fuel cruel and dangerous illegal wildlife trafficking.
Even within the WHO, there is tension over what is being platformed at the summit. One senior official, speaking on condition of anonymity, described homeopathy, a central pillar of Ayurveda, as “complete nonsense”.
“There is not one shred of evidence anywhere, absolutely anywhere, that suggests it works,” the official said, while acknowledging pressure to engage rather than alienate powerful member states. Ernst, the British-German academic, said: “Many experts are puzzled by this attitude. The most likely explanation is that the WHO is bowing to political will instead of science.”
Homeopathy is based on the principle of “like cures like” and claims to treat illness by administering highly diluted substances that, in undiluted form, would produce symptoms similar to those of the disease. For example, a homeopathic remedy might involve giving a highly diluted preparation of poison ivy – which can cause a red, itchy rash – to someone experiencing similar skin symptoms.
But even if you accept the principle of homoeopathy – for which there is no robust scientific evidence – the dilution of these “remedies” is so extreme that, more often than not, not a single traceable molecule of the original “healing” substance remains.
Ben Goldacre, a British doctor and professor of evidence-based medicine at the University of Oxford, who refers to homeopathic drugs as “empty little sugar pills”, explained in his bestseller book Bad Science: “The typical homeopathic dilution is 30C: this means that the original substance has been diluted by one drop in 100, 30 times over. The Society of Homeopaths’ website will tell you that 30C contains less than one part per million of the original substance.
“ ‘Less than one part per million’ is something of an understatement: a 30C homeopathic preparation is a dilution of one in 10 [to the power of 60], or one followed by 60 zeroes. For perspective, there are around 100,000,000,000,000,000,000,000,000,000 molecules of water in an Olympic-sized swimming pool. Imagine a sphere of water with a diameter of 150 million kilometres (the distance from the Earth to the sun) with one molecule of a substance in it: that’s a 30C dilution.”
At the heart of the debate lies a dilemma: how to assess traditional medicine by the same standards as Western medicine without compromising scientific rigour – and whether doing so is worthwhile at all.
“There are some alternative therapies that will have merit,” said Dr John Reeder, former head of the WHO’s tropical disease unit. “The benefit here is not to shift everybody to traditional medicine or vice versa. But if we as the WHO, for example, can say that yoga is beneficial in a post-operative patient, then that would be a good thing.
“It’s not about, ‘Do you have a traditional medicine solution or a Western medicine solution?’ It’s, ‘Are you as a patient getting the best available solution?’ And if you can get an equivalent relief of your problem with a traditional method that costs a fraction and you don’t have to go to the hospital – well, why wouldn’t you? That’s obviously better for you.”
Dr Lluis Vinyals Torres, director of the WHO’s Western Pacific region, said: “If we ignore traditional medicine, we are going to miss a huge chunk of people who are going to use it anyway. It makes sense to help countries enforce regulations, for example by stopping people from using herbal ingredients that aren’t safe.”
Globally, an estimated 4.6 billion people already use some form of traditional medicine. In sub-Saharan Africa, millions rely on traditional healers as their first – and sometimes only – point of care. Its use can delay access to appropriate treatment, and some practices have been linked to the spread of disease.
At least 41 people were reported to have died in the last two months of 2025 after undergoing rituals to initiate them into manhood in South Africa, a central part of which involves unsafe and brutal circumcisions. Another example, common in places like Uganda, Benin, and Burkina Faso, includes small skin incisions into which herbs are rubbed – sometimes referred to as “vaccinations” – increasing the risk of HIV transmission through the reuse of razors and knives.
Efforts to regulate practitioners are underway, but progress remains slow. Malawi’s Minister for Health and Sanitation, Madalitso Baloyi, said her government wanted clear guidance from the WHO: “As a ministry, we want to ensure [traditional remedies] are tested and quality checked.” She added that, at the moment, traditional medicine is being done “behind closed doors” and that the WHO process would help bring it into the open where it can be better monitored.
Alternative medicine is also booming across Europe and the United States – from homeopathy to supplements like the shrub ashwagandha, meditation and so-called lifestyle “hacks” such as drinking raw milk or avoiding suncream.
Earlier this month, US health secretary RFK jnr confirmed he had cut six federal vaccine recommendations from the childhood immunisation schedule – including jabs for meningitis, hepatitis and COVID-19. Dr Michael Osterholm, director of the University of Minnesota’s Centre for Infectious Disease Research and Policy, described the decision as “radical and dangerous”.
Yet the WHO seems undeterred. “Some traditional remedies will probably be found to be really active and really useful. Others will just be a placebo – for example, you feel better when you drink tea,” said Reeder.
The WHO argues that investing in traditional medicine could also help tackle the leading killers of the 21st century: non-communicable diseases such as obesity, diabetes, cardiovascular disease and mental illness. Holistic approaches to wellness incorporating exercise, a more considered diet and stress reduction could complement conventional treatments, placing “an emphasis on prevention over cure”, said Tedros.
To an extent, the WHO has been taking this approach already. In December, the organisation announced that it now recommends GLP-1s, which includes products like Mounjaro and Wegovy, as a worldwide treatment for obesity, but in combination with healthy diets and regular physical activity because, Tedros said, “medication alone won’t solve this global health crisis”.
Officials also point to a “treasure trove” of potential drug discoveries hidden in nature. About 40 per cent of modern pharmaceuticals are derived from plant compounds used in ancient remedies, according to Dr Shyama Kuruvilla, director of the WHO Global Traditional Medicine Centre.
Artemisinin, a frontline malaria treatment, was isolated from sweet wormwood, long used in Chinese medicine. “Now with technology we can analyse what is the real compound that is [inside traditional remedies] that has efficacy and look to isolate them,” said the WHO’s Briand. “By isolating it, we could take the best of it and not have the adverse effects that are linked to the rest of the plant, for instance.”
Last year, WHO member states approved a 10-year traditional medicine strategy committing the organisation to an “evidence-based” approach. At the summit, the WHO launched its traditional medicine library – an online database containing more than 1.6 billion records, from Inuit midwifery to tobacco-smoke enemas.
“This doesn’t mean we endorse anything,” Briand said. “It simply brings everything together so we can study it faster.”
“When we do produce guidelines, no unsafe practice will come out of WHO,” Torres, of the WHO’s Western Pacific region, added.
The difficulty lies in how evidence itself is defined. Western “biomedicine” emerged largely during the Industrial Revolution, when scientific advances allowed for rapid progress in preventing illnesses and understanding how bacteria and viruses operated.
The discovery of penicillin in the 20th century which brought with it the antibiotic revolution, the integration of laboratory sciences with medicine and the invention of vaccines all contributed to the field of modern medicine as we now understand it.

But even then, rigorous testing was not the norm. Randomised controlled trials (RCT) and systematic reviews only became widespread in the 1980s and 1990s and was the first time real rigour was applied to medicine. This was driven in large part by the work of the Cochrane Collaboration, an organisation started in Britain that champions the use of double-blind RCTs – the gold standard of evidence. The shift towards RCTs overturned many long-accepted Western medical practices, including the recommendation of cough syrup for coughs and colds, valium for depression and cranberry juice for urinary tract infections.
But applying this framework to traditional medicine across the globe to decipher what is actually effective presents a huge challenge. “Take yoga,” said Reeder. “How do you design a placebo for yoga? People say they feel better – but anecdotes aren’t evidence.”
Briand, the WHO’s chief scientist, said the organisation is investing in building a previously non-existent evidence base for ancient practices, using technologies such as artificial intelligence, genomics and brain imaging. “For example, we had a session [at the summit] on meditation, and it shows that, with brain imagery, meditation is modifying the grey matter in the brain,” she said. “This is a very concrete outcome of this practice that before was not proven. This is the kind of work that we can do now that we couldn’t do 50 years ago.”
Reeder said alternative therapies would only be endorsed if they could meet the same evidentiary standards. “If you show us the evidence, show us the proof, we’ll really consider [endorsing therapies]. People coming in here with homeopathy are getting their platform, but unless they come up with the evidence that it’s needed, it isn’t going to work.”
Cochrane has a dedicated group to examine how traditional medicine can be tested to a high standard. Now, Dr Susan Wieland, director of Cochrane’s complementary medicine team, is supporting the WHO as co-chair of its new strategic advisory group on traditional, complementary and integrative medicine that will give technical advice to the organisation as it goes through this process, which was launched at the Delhi summit.
“Cochrane itself is moving beyond just randomised controlled trials. They also look at questions of prognosis, very complex interventions, and qualitative research,” said Wieland. Incongruously, she co-chairs the new steering group alongside Professor Martins Emeje, a man who believes that “the plants, the animals, the soil and the marine life of [a] community” are capable of preventing diseases like diabetes and malaria.
Weiland added that Cochrane’s work with the WHO on traditional medicine reflects “an opening up and a desire for collaboration and connection between different regions of the world, policymakers, researchers, clinicians and different traditions”.
But, at the summit, there are still more questions than answers for the moment at least. That tension defines the WHO’s gamble. Some traditional remedies will almost certainly prove useful. Many will not. Separating the two – while resisting political pressure and commercial lobbying – may be one of the most difficult balancing acts the WHO has ever attempted.
Whether this push becomes a global health breakthrough or a costly detour will depend on whether science, rather than belief, ultimately sets the rules.
This is an edited version of a story that first appeared in The Telegraph (UK).
Get the best of Good Weekend delivered to your inbox every Saturday morning. Sign up for our newsletter.